What is HbA1c and what’s the HbA1c normal range?
Last updated
Key Article Takeaways
- HbA1c is an estimate of your average blood sugar levels over the last 2-3 months.
- The pre-diabetes HbA1c range is 39-47mmol/mol
- The diabetes HbA1c level is 48mmol/mol and above
- But you really need to be aiming for an optimal HbA1c range of 30-35mmol/mol
How your body handles your blood sugar levels is a fundamental part of your metabolic health. In turn, metabolic health impacts everything from your risk of diabetes, heart disease, cancer and death1. Ok, so how do you measure your sugar-handling?
HbA1c is a quick and easy blood test you can do at home is one of the commonest ways to measure how your body is handling your blood sugar. But what is HbA1c, how does it measure your blood sugar levels and what’s the HbA1c normal range? We’ll also cover the pre-diabetes HbA1c and diabetes HbA1c levels.
What is HbA1c?
HbA1c or “haemoglobin A1c” is a type of haemoglobin that has a sugar molecule stuck to it. This is called “glycated haemoglobin”. Haemoglobin is a protein found in your red blood cells (RBCs) that carries oxygen. The more sugar you have in your blood, the higher your level of glycated haemoglobin or HbA1c.
So HbA1c is a way of estimating your average blood glucose concentration. It’s important to stress that it’s an estimate because HbA1c doesn’t measure your blood glucose directly but infers it from the amount of glycated haemoglobin in your blood.

The other important thing to know about HbA1c is that it’s an estimate of your average blood sugar levels over the last 2-3 months. Why’s this? Well, haemoglobin is carried in your RBCs and your RBCs last in your circulation for about 90 days. So when we measure HbA1c, we’ll be measuring it on RBCs that are brand new as well as RBCs that are 90 days old.
How do we measure and report HbA1c?
We can measure HbA1c from a simple blood test and you’ll see results reported in two ways. In the UK, we generally report HbA1c as the amount of glycated haemoglobin per amount of total haemoglobin using the “International Federation of Clinical Chemistry” units “mmol/mol”.
You might also see an older way to report HbA1c as a percentage of glycated haemoglobin out of the total amount of haemoglobin. This is known as the Diabetes Control and Complications Trial units and is still common in the USA.
What is the HbA1c normal range?
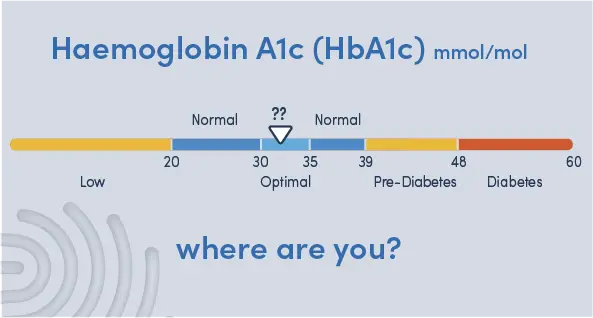
The HbA1c normal range is from 20 to 39mmol/mol (4 to 5.7%) and is the same for everyone, regardless of age or sex. However, there’s actually a bit more to it than that.
You need to think of HbA1c as a continuum from good to poor sugar-handling. At various points along this continuum, people have somewhat arbitrarily slapped labels like “normal, “pre-diabetes” and “diabetes”. For example, in the USA, pre-diabetes is defined as an HbA1c of 39 to 47mmol/mol2. In contrast, in the UK someone isn’t considered pre-diabetic until their HbA1c gets up to 42mmol/mol3.
When it comes to full-blown diabetes, the USA and UK agree that 48mmol/mol and above is the cut-off but what if you’re at 47mmol/mol? Are you really that different from someone with an HbA1c of 48mmol/mol? Does your risk suddenly change? Did you suddenly go from not having a disease to having a disease that needs treatment? Of course not - it’s arbitrary.
What we can all agree on is that, in general, lower is better. It’s better to have an HbA1c of 38 than 40mmol/mol even if those levels would both be considered “normal” in the UK. That’s why we use the American definition of pre-diabetes at Selph - it’s more conservative and we don’t believe you should consider an HbA1c of 39 to 41mmol/mol to be “normal”.
| HbA1c (mmol/mol) | HbA1c (%) | Diagnosis |
| under 20 | under 4 | Low |
| 30 - 35 | 5 - 5.4 | Optimal |
| 20 - 38 | 4 - 5.6 | Normal |
| 39 - 47 | 5.7 - 6.4 | Pre-diabetes |
| 48 and above | 6.5 and above | Diabetes |
What is an optimal HbA1c?
Remember that when it comes to “normal”, lab tests generally use a range that includes 95% of the population. In the UK, almost three quarters of the population aged 45 to 74 are overweight or obese4, 1-in-4 people die of heart disease5 and 1-in-4 die from cancer5. Being “normal” is really not something we should strive for if we want to live a long and healthy life.
Data have shown that the risk of dying from any cause, dying from cancer or dying from cardiovascular disease all go up once your HbA1c goes over the “normal” value of 36.6mmol/mol or 5.5%1. That’s why we suggest that an optimal HbA1c level should be between 30 and 35mmol/mol.
Fortunately, your HbA1c level is under your control to a large degree. Our experts have gone through the latest evidence to bring you 7 science-backed tips to optimise your HbA1c level.

Why a very low HbA1c may not be “healthy”?
Various studies have shown that once you get to an HbA1c below about 30mmol/mol or 5%, mortality actually goes up6. It’s worth noting that an HbA1c of 20-30 is still considered “normal”. How does that work you might ask? Well, it’s probably nothing to do with sugar-handling but rather related to other conditions that can cause a low HbA1c such as malnutrition, red-blood cell problems, liver issues or the early stages of chronic disease6. So a low HbA1c can be a sign that something else is going on that’s bad for your health.
We use an HbA1c of 30mmol/mol as the lower end of our “optimal” range. That’s not to say that if you’re a little below this you should try to raise your HbA1c! It may just be that you’re very slim but perfectly healthy. However, if your HbA1c is far below 30mmol/mol, it would be sensible to consider if there’s a specific reason for this.
When might your HbA1c be “wrong”?
Remember that HbA1c is just an estimate of your average blood sugar for the last 2-3 months. While the HbA1c number itself can’t be “wrong” (unless there was a problem with the analyser), in some cases it might not be a good estimate of average blood sugar.
For example, anything that affects how quickly red blood cells are removed from your circulation will affect HbA1c. This is because sugar builds up on haemoglobin over time so the longer the RBCs circulate the higher the HbA1c will be, even for the same average glucose concentration. Conditions where RBCs are removed more slowly from the circulation, like iron deficiency anaemia, will tend to raise HbA1c where as conditions where RBCs are removed more rapidly can do the opposite7.
In general though, HbA1c is a pretty good predictor of average blood sugar and you can certainly rely on it to tell you “directionaly” if your sugar-handling is getting better or worse based on the level going up and down.
How else can you check your average blood sugar?
It used to be pretty tough to know your average blood sugar but continuous glucose monitors (CGMs) have changed all that. These small wearable devices measure the glucose levels in the fluid between cells which can be used to quantify blood sugar with a very high accuracy8. The device pairs with a smartphone app so you can monitor your blood glucose in real-time and see the effects of food, sleep, exercise and stress on your blood sugar. You can also look at trends over time such as average, variability and peaks; all of which give you unique insights into sugar-handling beyond what HbA1c can tell you.

At Selph, we regularly use CGMs with our clients to get a more accurate, personalised assessment of their sugar-handling and aid in making a plan to optimise their levels. Our CGM programme includes the use of the sensor for two weeks, a glucose challenge, a consultation with one of our experts and written report and plan. Find out more about our CGM programme.
Get tips on better health
Sign up to our emails on the better way to better health.
We'll keep you up-to-date with the latest research, expert articles and new ways to get more years of better health.








