What is a continuous glucose monitor (CGM) and what can a non-diabetic learn from one?
Published
Key Article Takeaways
- A continuous glucose monitor (CGM) gives you real-time feedback on your blood glucose levels.
- Metabolic health or disease is one of the key drivers of diabetes, heart disease, dementia, cancer and ageing.
- How your blood glucose responds to your environment - food, exercise, sleep & stress - is a key read-out of your metabolic health.
- CGMs provide a "window" to assess your metabolic health and help guide optimisation.
A Continuous Glucose Monitor or CGM is a small wearable device that measures your blood glucose level and sends the data to your smart phone for you to see in real-time.
CGMs were developed to provide an easy way for people with diabetes to know their blood sugar levels without resorting to uncomfortable finger-pricks multiple times a day. However, their ease of use has also made them accessible to people without diabetes who want to take a closer look at their blood sugar levels.
But if you don’t have diabetes, why would you care about knowing your blood sugar levels in real-time? What can the levels tell you and why is it important?
How does a CGM work?
A CGM has a tiny filament (about the width of dental floss) that sits under the skin, in contact with the “interstitial” fluid that bathes cells. The filament is coated in an enzyme called glucose oxidase which breaks down glucose. As glucose is broken down, molecules produced by the reaction generate a minute current in the sensor that can be converted into a glucose reading.
Strictly speaking, a CGM measures the glucose concentration in the interstitial fluid, rather than the blood. However, the two are in equilibrium so interstitial glucose concentration provides a very good approximation of blood glucose. There is a lag of about 10-15 minutes while the glucose in the blood equilibrates with the interstitial fluid but this is inconsequential for our purposes.
What does a CGM tell you?
The CGM biosensor will record your glucose level over time and send it to an app on your phone over bluetooth. In the app, you’ll be able to see your blood glucose plotted over time.
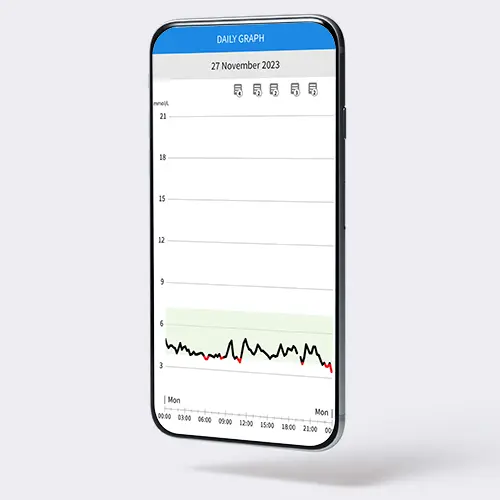
As you go about your day, eating, exercising, sleeping… you’ll be able to see how your glucose level fluctuates. How did that croissant, coffee and orange juice for breakfast affect your blood sugar? What if you worked out beforehand? What about if you had a bad night’s sleep? Or swapped the croissant for porridge?
Over time, you’ll build up a picture of how your blood sugar responds to your lifestyle. In particular, you’ll be able (with some help from Selph) to calculate some important metrics:
- Your average blood sugar
- Your fasting blood sugar
- How much variability there is in your blood sugar
- How often you’re getting significant spikes and how high those spikes go
Ok, so why should I care about these numbers if I don’t have diabetes?
We need to look at the bigger picture for a moment. 1-in-4 of us will die from heart disease, 1-in-4 from cancer, 1-in-3 will develop dementia,1-in-4 will have a stroke and half of adults over 65 are classed as “frail”.
One of the main drivers of all of these conditions is metabolic health. You can think of metabolic health as the end-product of the interactions between your genes, your environment (e.g. diet and exercise) and your gut microbiome. These three factors ultimately dictate all the reactions going on in your body - your metabolism.
Glucose is at the centre of your metabolism. It’s the preferred source of energy for your central nervous system (which can also use ketones) and, along with fat, is one of major sources of energy for your muscles. Given its importance, you have many complex, interconnected mechanisms to increase and decrease your blood sugar. When these glucose control mechanisms go awry you get something called “insulin resistance”.
Roughly 40% of adults are insulin resistant and insulin resistance precedes the development of type 2 diabetes by 10 to 15 years1. What’s more, we see insulin resistance in lean, non-obese people in their 20s2. This is not something that just affects other, older people. Insulin resistance affects people like you and has a profound influence on your risk of disease as you age.
Your glucose responses, as measured by a CGM, give us a window into this crucial aspect of your metabolic health. Failure to control glucose adequately after eating, large frequent glucose spikes and high variability in blood sugar all indicate sub-optimal metabolic health decades before diabetes or heart disease develops.
So, does a CGM just tell me what food to eat and what to avoid to keep my blood sugar low?
A CGM is absolutely NOT about telling you what to eat and what to avoid. Let’s be honest with ourselves; we don’t need a fancy biosensor to tell us that cake is going to raise our blood sugar!

Yes, you will almost certainly get some surprises about foods which raise your blood sugar more than expected (grapes anyone!) but by and large, the aim is not simply to replace these with foods that don’t raise your blood sugar.
Remember, glucose responses are just one aspect of your metabolic health. Switching porridge for bacon every morning is not likely to be a sensible health choice even though it may make your glucose look good!
Blood glucose is just one read-out of your metabolism. Food goes in, metabolism happens and blood glucose is our output. Food is undoubtedly important but we should care more about the metabolic engine in the middle. A metabolically healthy person can eat a slice of cake, have a low spike in glucose that’s rapidly cleared. A metabolically unhealthy person will have a larger spike and take longer to get back to baseline. The problem isn’t the cake per se (assuming you’re not eating it every day!); the problem is your metabolic health. A CGM can give you this insight into your metabolic health. Then you can go away and put in some time to “retune” your metabolic engine before retesting with a CGM to see how far you’ve come.
Are there any risks or harms associated with using a CGM?
CGMs are safe medical devices and, from a physical perspective, about the worst that can happen is that you can get a skin reaction to the adhesive used to hold the sensor on.
However, a more important potential issue is that using a CGM could provoke feelings of anxiety around eating. This may simply be unpleasant but has the potential to be more significant if someone has an eating disorder. We don’t really have data to suggest that this is a widespread problem but we haven’t been using these devices for long in non-diabetics so it’s certainly plausible.
More generally, as I’ve mentioned above, there could be a tendency to try and “beat the system” by adopting food choices that lower your glucose but aren’t necessarily beneficial for your health overall. There’s more to you and your health than just blood glucose. To some degree common sense has a role to play here. However, I think it’s also an area where guidance from experts can help you understand how to optimise your metabolism for the long-term.
Get tips on better health
Sign up to our emails on the better way to better health.
We'll keep you up-to-date with the latest research, expert articles and new ways to get more years of better health.


