What is non-coeliac gluten sensitivity and how do I know if I have it?
Medical review by
Dr Alasdair Scott MBBS FRCS PhDLast updated
Key Article Takeaways
- Non-coeliac gluten sensitivity is an intolerance to gluten-containing foods.
- You might have it if you get bloating, cramping and stomach pain after eating bread, pasta or pastries.
- Coeliac disease and Helicobacter pylori infection have similar symptoms, so rule them out with our Coeliac and H. pylori Combined Test for Indigestion.
- To find out if you have non-coeliac gluten sensitivity, you’ll need to do a placebo-controlled “gluten challenge”.
Do bread, pasta or cakes give you unpleasant symptoms like feeling bloated, sick or having stomach pain? Non-coeliac gluten sensitivity might be to blame but other conditions can have similar symptoms. We’ll explain the differences between coeliac disease, wheat allergy and non-coeliac gluten sensitivity. We’ll also cover their symptoms and how you can figure out if one of them is affecting you, including the tests you can take.
First things first, what is coeliac disease?
Coeliac disease is an autoimmune condition where your body reacts to gluten in your diet. Gluten is a protein in wheat (used to make flour), barley and rye so you’ll find it in bread, pasta, beer and pastries. Gluten triggers your immune system to attack the lining of your gut, causing inflammation and symptoms such as bloating, stomach pain and diarrhoea. The gut inflammation also makes it harder to absorb nutrients from food which, over time, can lead to weight loss and vitamin deficiencies.
We have a whole article on coeliac disease where we delve into what causes the disease in more detail and cover everything you need to know about testing for it.
Ok, and what about wheat allergy?
Some people can actually be allergic to wheat in the same way that people can be allergic to peanuts. They’ll get an allergic reaction minutes to hours after eating wheat-containing foods. Tell-tale symptoms of wheat allergy are irritation or swelling of the lips, tongue and throat and itchy, red rashes (“hives”). In more serious cases your breathing can get wheezy or difficult.

What’s the difference between coeliac disease, wheat allergy and non-coeliac gluten sensitivity?
Non-coeliac gluten sensitivity is a food intolerance, where foods containing gluten can give you uncomfortable symptoms. It’s also called non-coeliac wheat sensitivity as it’s often foods containing wheat that are a particular trigger. However, unlike wheat allergy, it is not an allergic reaction that causes swelling or itching. Neither is it an autoimmune disease where you have painful gut inflammation. Non-coeliac gluten sensitivity doesn’t cause an immune response and there is no damage to your gut lining.
While it is called “gluten” sensitivity, it is not absolutely certain that the symptoms are actually caused by the gluten part of wheat1. Some scientists have suggested that other parts of wheat or even other nutrients that are commonly found within wheat-containing foods could be to blame. The absence of a clear disease process has made it challenging for experts in the field to arrive at a clear definition for this condition.
What are the symptoms of non-coeliac gluten sensitivity?
The symptoms of non-coeliac gluten sensitivity can be a little vague and everyone has a different experience. You might notice bloating, stomach pain, nausea or diarrhoea after you eat foods containing gluten. People also describe headaches, tiredness, joint pain and “brain fog” or difficulty concentrating.
Some of these symptoms, like bloating and stomach cramps, overlap with coeliac disease and wheat allergy so it can be hard to distinguish between these conditions based on their symptoms. Wheat allergy will tend to cause symptoms very quickly and the rash and swelling around the mouth will be the main symptoms. Coeliac disease is tougher to distinguish from non-coeliac gluten sensitivity but if you’re experiencing weight loss and/or vitamin deficiencies, then coeliac disease is much more likely. The best way to tell for sure is to do a blood test for coeliac disease.

I think I might have non-coeliac gluten sensitivity - what should I do?
First off, make sure it’s not coeliac disease or Helicobacter pylori infection
If you’re wondering if you might have non-coeliac gluten sensitivity the first thing to do is rule out other conditions that cause similar symptoms. This is important because other conditions, such as coeliac disease or H. pylori infection (more on that later), can cause serious complications if you don’t pick them up and they go untreated.
It’s easy to test yourself for coeliac disease with our Coeliac Disease Gluten Sensitivity Test. This is a simple finger-prick blood test that you can do at home and post to our lab. You’ll get your results back within only a few days. We’ve written an in-depth article on blood tests for coeliac disease that will be helpful.
Helicobacter pylori is a common bacteria that can infect your stomach and cause indigestion symptoms - bloating, pain or discomfort after eating. Again, we’ve got a great article all about H. pylori, the symptoms it causes and how to test for it. Because H. pylori infection and coeliac disease can mimic each other, we’ve created our Coeliac and H. pylori Combined Test for Indigestion so you can test for both of them at the same time.
Ruling out coeliac disease and H. pylori infection are key first steps, but that still doesn’t mean you’ve got non-coeliac gluten sensitivity.
Do a “placebo-controlled gluten challenge”
Many of the foods that contain wheat and gluten such as breads, cereals and snacks, also contain other substances that we know can trigger symptoms in people with irritable bowel syndrome. If you just stop eating gluten-containing foods, you’ll also cut out all the other things these foods contain. So how will you know it’s actually the gluten you’ve got a problem with and not something else? You need to do a placebo-controlled gluten challenge2.
In a placebo-controlled gluten challenge, you take pills that contain either gluten or a “placebo”. Both the pills look and taste the same but the placebo pills don’t have gluten and have no effect on your body. You keep track of any symptoms you get while taking each pill for about a week but you won’t know if you’re taking the gluten or the placebo. This is important because if you know you’re taking the gluten pills it can affect the symptoms you experience.
At the end of the challenge we can reveal which pills were which and compare the symptoms you experienced on the placebo versus the gluten pills. If you had more severe symptoms with the gluten pills then it’s likely you have non-coeliac gluten sensitivity. If this sounds a little complicated to imagine, we’ve drawn out how the challenge works in figure 1 below.
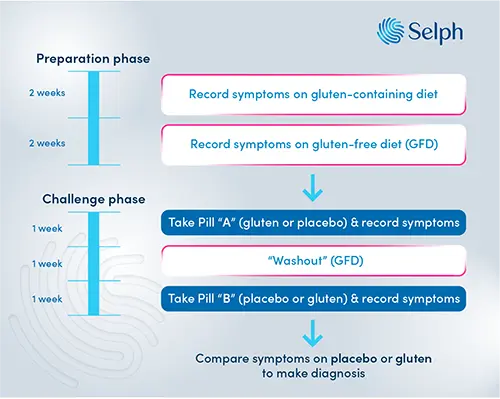
Why is it important to diagnose non-coeliac gluten sensitivity?
So, why bother going to the effort of making sure that gluten is the culprit? Why not just cut out all foods containing gluten and be done with it? Contrary to popular opinion, gluten is not harmful to most people. In fact, gluten is in lots of very “nutrient-dense” foods. Basically, it's in a lot of things that are good for you! If you cut out gluten you’re missing out on these nutritious foods and rather than benefiting your health, studies have shown that you can actually be doing yourself harm. For example, gluten is in many “whole grains” which have well-proven benefits to heart health. If you avoid these foods unnecessarily you may increase your risk of getting coronary heart disease3.
Going gluten-free is absolutely required if you have coeliac disease and may also be necessary if you have a proven sensitivity to gluten. But otherwise, a gluten-free diet has no proven health benefits at best, and at worst, may actually be harmful. Not only that, but it’s a huge lifestyle shift to go gluten-free and is very difficult for most people.
Putting in the effort to make sure that you don’t have coeliac disease and that gluten is actually the cause of your symptoms is absolutely worth it.

Get tips on better health
Sign up to our emails on the better way to better health.
We'll keep you up-to-date with the latest research, expert articles and new ways to get more years of better health.


